 Poor performance status (PS ≥2) and high karyotype risks in IPSS-R (high and very high) were significant risk factors of death and AML-progression in Cox proportional hazards analysis.Ībstract = "Hypoplastic myelodysplastic syndrome (hMDS) is a distinct entity with bone marrow (BM) hypocellularity and the risk of death from BM failure (BMF). In competing risks analysis, hMDS exhibited decreased risk of AML-progression in lower IPSS or IPSS-R risk patients, and higher risk of death from BMF in patients at age ≥50. The overall survival (OS) and AML progression-free survival (AML-PFS) of hMDS were higher than those of non-hMDS, especially in patients at age ≥50 and of lower risk in Revised International Prognostic Scoring System (IPSS-R). More RA and fewer CMMoL and RAEB-t in French-American-British (FAB) and more RCUD and MDS-U and fewer RCMD in World Health Organization (WHO) classifications were found in hMDS than non-hMDS with significant differences. 
To elucidate the characteristics of hMDS, the data of 129 patients diagnosed between April 2003 and March 2012 were collected from 20 institutions and the central review team of the National Research Group on Idiopathic Bone Marrow Failure Syndromes, and compared with 115 non-hMDS patients. After diagnosed by morphology and cytogenetics especially molecular genetic information may therefore guide treatment in the near future for this low risk subgroup of MDS patients as investigated here.Hypoplastic myelodysplastic syndrome (hMDS) is a distinct entity with bone marrow (BM) hypocellularity and the risk of death from BM failure (BMF).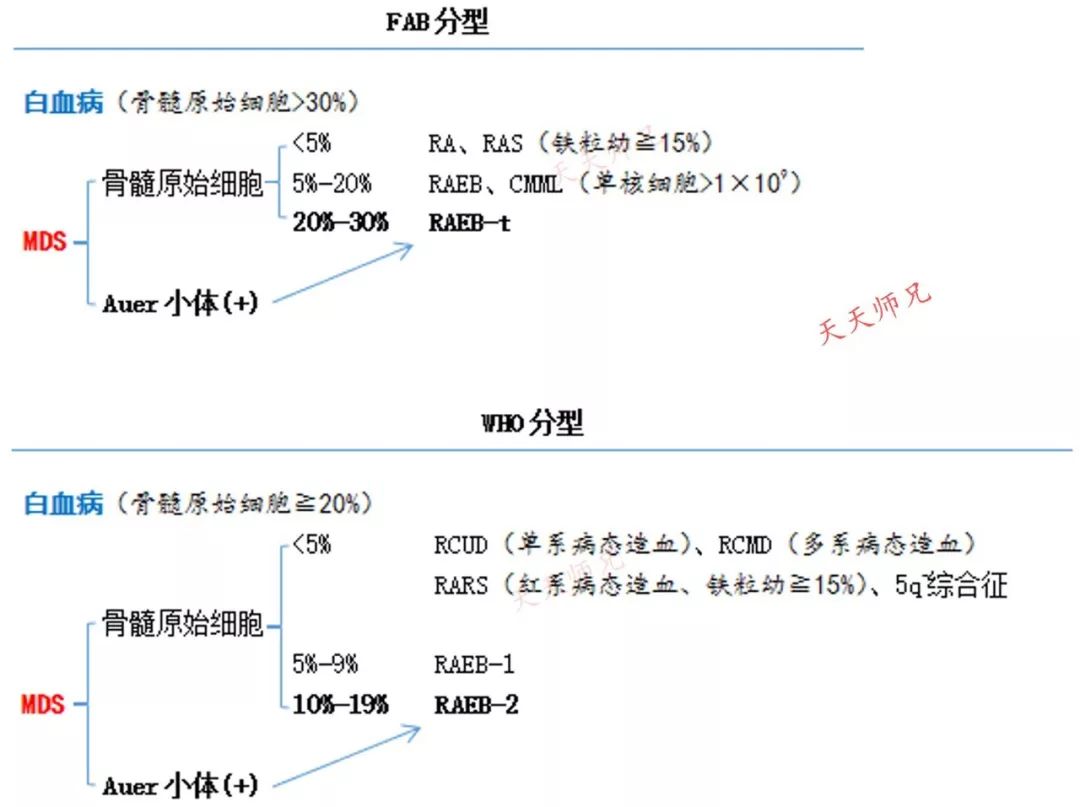 
To overcome this shortcoming only an increasing panel of new molecular markers in MDS can pave future investigations which presently becomes available by the advanced sequencing techniques. Mean WBC count differed between all subgroups (RARS: 6.1 RCMD: 4.4 RCMD-RS: 5.3×10(9)/l RARS vs RCMD p80% of patients show a good risk cytogenetic profile making prognostication according to karyotype relevant only in a small subset of patients. Mean age (RARS: 71.8 RCMD: 70.1 RCMD-RS: 72.6 yrs) reached significant difference between RARS vs RCMD (p=0.020) and between RCMD vs RCMD-RS (p=0.004). Results: Sex ratio (male preponderance in all subtypes male/female ratio 1.9 in the whole cohort) did not differ significantly between the 3 MDS subgroups. Cytogenetic risk groups were defined according to the International Prognostic Scoring System (IPSS Greenberg et al., 1997). Study Design: To investigate the clinical impact and genetic background of these MDS subtypes, we studied outcomes, cytogenetics, and molecular genetics in 1082 de novo MDS pts (153 RARS, 606 RCMD, 323 RCMD with ring sideroblasts ≥15% termed “RCMD-RS“): 703 m/379 f median age, 73.1 yrs 21.0–90.4 yrs. One aim of this study was to evaluate whether or not a separation with respect to ring sideroblasts is reasonable. 
In 2008 the WHO classification combined the former categories RCMD (refractory cytopenia with multilineage dysplasia) and RCMD-RS (with ring sideroblasts ≥15%) thus not separating according to ring sideroblasts anymore in MDS with multilineage dysplasia, while the category refractory anemia with ring sideroblasts (RARS) was maintained separately. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
